Bone-Conduction Hearing Aids: A Guide to Alternative Amplification
 Apr, 24 2026
Apr, 24 2026
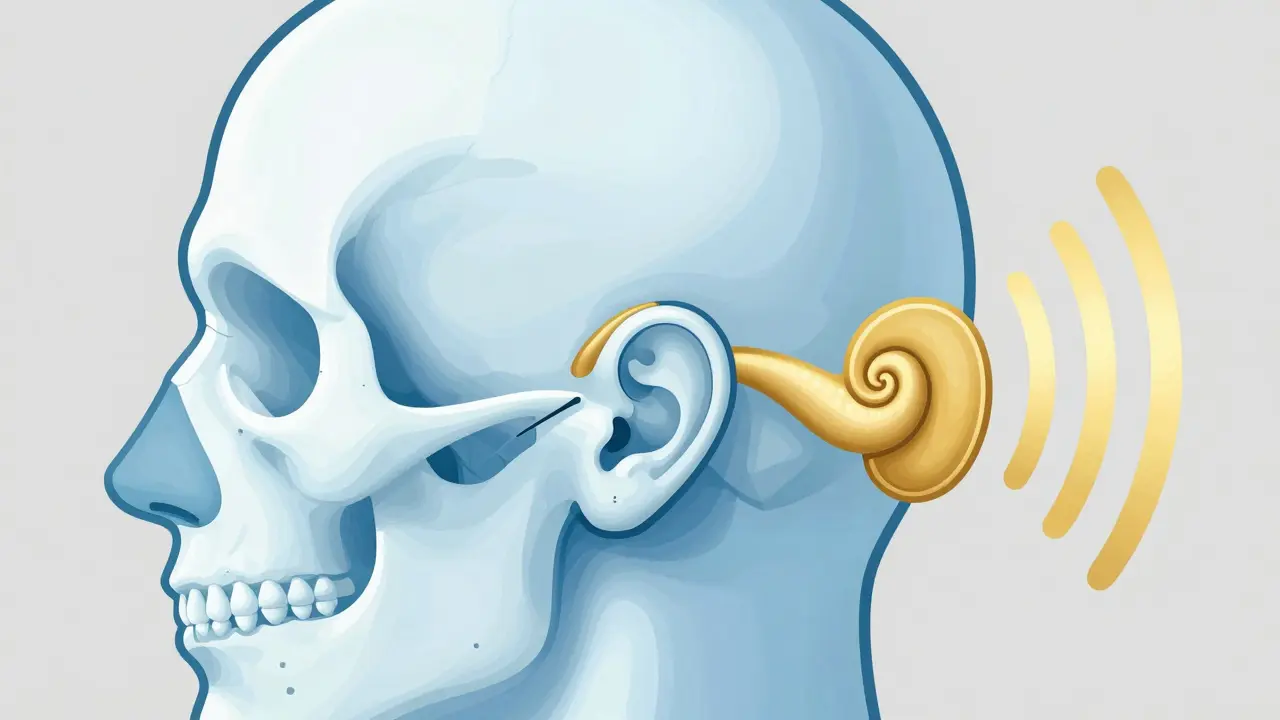
Imagine waking up and realizing that the way you experience sound isn't about what enters your ear canal, but what vibrates through your skull. For most of us, hearing is a simple process: sound waves hit the eardrum and travel through a series of tiny bones to the inner ear. But for people with chronic ear infections, congenital malformations, or deafness in just one ear, that path is blocked. This is where bone-conduction hearing aids is a specialized hearing technology that transmits sound vibrations directly through the skull bone to the cochlea, bypassing the outer and middle ear structures entirely. It isn't just a different brand of hearing aid; it's a completely different way of getting sound into your brain.
How Bone Conduction Actually Works
Traditional hearing aids are like megaphones for your ear canal-they make the air vibrations louder. Bone conduction, however, turns sound into mechanical vibrations. These vibrations travel through the temporal bone of your skull. While it sounds strange, your body has several pathways to make this happen. Research from Linköping University shows that about 60% of this process comes from the inertia of the fluids inside your cochlea, while the rest comes from the compression of the cochlear walls and the movement of the middle ear bones.
Essentially, these devices skip the "broken" parts of the ear. If you have a blockage in the outer ear or a damaged eardrum, it doesn't matter. The vibration goes straight to the Cochlea the spiral-shaped cavity of the inner ear that transmits nerve impulses to the brain , which then tells your brain you're hearing a conversation, a song, or a bird chirping.
Who Should Consider This Alternative?
You can't just walk into a store and buy these; they are medical solutions for specific types of hearing loss. If you have a standard age-related hearing loss (sensorineural), these likely won't help you much. But they are a game-changer for three specific groups:
- Conductive Hearing Loss: When sound can't get through the outer or middle ear. For people with congenital aural atresia (being born without an ear canal), these devices have a success rate of 85-90%.
- Single-Sided Deafness (SSD): When one ear is completely deaf. Bone conduction allows sound from the "dead" side to be sent across the skull to the functioning ear, helping you locate where sounds are coming from.
- Chronic Ear Infections: If your ears are constantly infected, putting a plug in your ear canal can make things worse. In about 92% of these cases, traditional aids are contraindicated, making bone conduction the only safe option.
Percutaneous vs. Transcutaneous Systems
When you look into these devices, you'll find two main styles: those that go through the skin and those that stay under it. Choosing between them usually comes down to a trade-off between sound power and aesthetics.
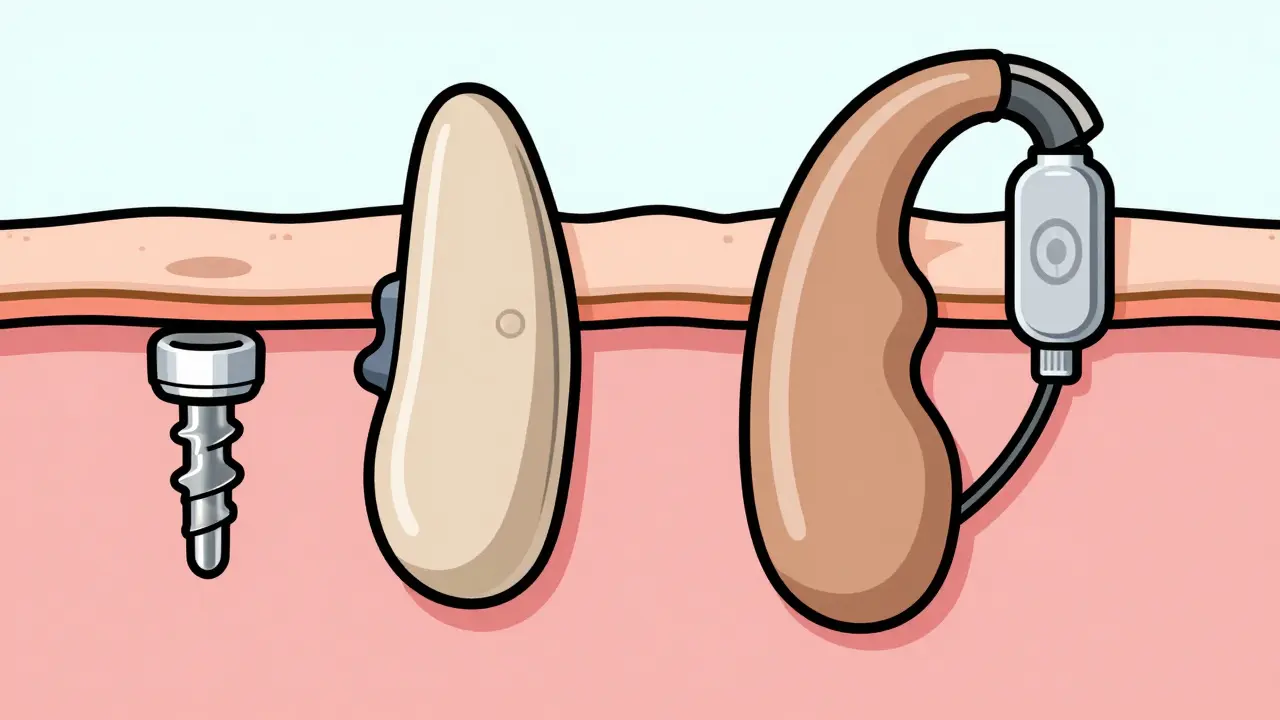
The percutaneous systems, such as the BAHA Bone-Anchored Hearing Aid, a system where a titanium implant is surgically placed in the skull , use a titanium abutment that sticks out through the skin. The sound processor snaps onto this post. Because there is no skin in the way, the sound is crisp and powerful, often providing up to 50 dB of gain. The downside? About 28% of users experience skin irritation around the post, and you have to clean it daily with 70% isopropyl alcohol to keep infections away.
Transcutaneous systems, like the Bonebridge a transcutaneous bone conduction implant that uses magnetic coupling to transmit sound through the skin , are entirely hidden. A magnet is implanted under the skin, and the processor snaps on via magnetic force. These are far more discreet-92% of users prefer the invisible look-but they lose some power. Because the sound has to travel through a few millimeters of skin and soft tissue, you lose about 10-15 dB of signal compared to the "post" version.
| Feature | Percutaneous (Abutment) | Transcutaneous (Magnetic) |
|---|---|---|
| Visibility | Visible post on skin | Completely hidden |
| Sound Power | Higher (up to 50 dB gain) | Lower (max 45 dB output) |
| Skin Issues | Higher risk of irritation | Very low risk |
| Recovery | 3-4 months for integration | Immediate use possible |
| Hygiene | Requires daily cleaning | Standard skin care |
The Cost and Surgical Reality
Let's be real: this isn't a cheap or easy path. While a premium traditional hearing aid might cost you between $1,500 and $3,500, a bone conduction implant typically runs between $4,000 and $7,000 per ear. You're paying for the surgery, the titanium implant, and the specialized processor.
The surgery itself is usually a minor outpatient procedure. You're under local anesthesia for about 30 to 60 minutes. If you get a percutaneous system, you have to wait a few months for osseointegration-that's when your bone actually grows into and fuses with the titanium implant. If you go the magnetic route, you can often start using the device much sooner.
One big warning: if you need an MRI, check your device. Many of these implants are incompatible with high-strength MRI machines (1.5T+), and some users have reported the frustration of needing surgical removal or specific precautions before a scan.
Comparing Bone Conduction to CROS Systems
If you have single-sided deafness, you might also hear about CROS hearing aids Contralateral Routing of Signal aids that transmit sound from the deaf side to the good ear via a wireless link . CROS systems are non-surgical and easier to get, but they are basically just "shipping" the sound wirelessly. Bone conduction feels more natural. Studies show that bone conduction provides 15-20 dB better speech reception thresholds and significantly better sound localization, meaning you can actually tell where a car is coming from rather than just knowing there is a car somewhere.

Looking Ahead: AI and Full Implants
The tech is moving fast. We are seeing a huge shift toward magnetic systems, which now make up about 63% of new implants. Why? Because people hate dealing with skin sores and visible posts. New releases, like the BAHA 6 Max, now include Bluetooth 5.3 and 30-hour batteries, making them feel less like medical devices and more like high-tech gadgets.
The next frontier is the fully implantable device. Companies like Sonova are testing systems where there is absolutely nothing outside the skin-no processor snapping on, no magnets. Everything happens inside your head. This would eliminate the skin issues and the aesthetic concerns entirely.
Will bone conduction help me if I have nerve damage in my inner ear?
Generally, no. Bone conduction bypasses the outer and middle ear, but it still relies on the cochlea and the auditory nerve to function. If you have severe sensorineural hearing loss where the cochlea itself is damaged, bone conduction won't provide much benefit. It's designed for conductive or mixed hearing loss.
How long does the surgery take and is it painful?
The procedure is typically an outpatient surgery lasting between 30 and 60 minutes. It is performed under local anesthesia, so you shouldn't feel pain during the process. Most people return to their normal routine within 48 hours, though the "waiting period" for the bone to fuse with the implant (osseointegration) can take a few months for percutaneous models.
Do I have to clean the implant?
If you have a percutaneous system with an abutment (the post), yes. You need to clean the area daily, usually with 70% isopropyl alcohol, to prevent skin infections. Transcutaneous (magnetic) systems do not require this specialized cleaning since the implant is fully under the skin.
Can I get an MRI with a bone-anchored hearing aid?
It depends on the specific model and the strength of the MRI. Many implants are incompatible with 1.5T or 3T scanners. You must inform your radiologist about your implant, as some may require the external processor to be removed, and in some rare cases, the implant itself might need to be addressed.
Is it better than a standard hearing aid?
It's not necessarily "better," but it is "correct" for certain conditions. For someone with a blocked ear canal or chronic infections, a standard hearing aid is often useless or even dangerous. In those specific cases, bone conduction is far superior, offering 25-40% better speech understanding in noise.
Next Steps and Troubleshooting
If you suspect you have a conductive hearing loss, your first step is a comprehensive audiogram and a consultation with an ENT (Ear, Nose, and Throat specialist). Be sure to ask about "mixed hearing loss" if you feel a standard aid isn't doing enough.
For new users, expect a learning curve. Your brain has to get used to sound coming through your bones rather than the air. Audiologists typically recommend 2-4 weeks of auditory training. If you notice redness or discharge around a percutaneous abutment, don't wait-contact your surgeon immediately, as this could indicate a skin reaction or infection that requires antibiotics or revision surgery.
Ben Jima
April 25, 2026 AT 15:47This is a fantastic breakdown of the tech! For anyone on the fence, just remember that the initial recovery period is a small price to pay for the quality of life improvement. It's all about taking that first step and consulting a professional to see which path fits your specific biology.
Daniel Runion
April 26, 2026 AT 18:42Typical... just another way to push expensive surgeries!!! Why is the 10-15 dB loss for magnetic systems just "ignored" as a trade-off??? It's a huge deal!!!!
James Harrison
April 28, 2026 AT 00:59Makes you wonder how we define "hearing" anyway. It's wild that we can just reroute the signal through the skull. It's like a hardware bypass for the human body.
Brittney Prince
April 29, 2026 AT 13:32Sure, the "science" says it's great, but imagine what they're actually putting in your head. Titanium is one thing, but these "smart" processors with Bluetooth? Totally just a way for companies to track your brain waves and collect data from the inside out. Wake up people.
Nikita Shabanov
May 1, 2026 AT 01:15Actually, the distinction between conductive and sensorineural loss is critical here. Many people mistake one for the other during early self-diagnosis, which is why the audiogram mentioned at the end is the most important part of the whole process.
Sharyl Foster
May 1, 2026 AT 04:24CROS systems aren't just "shipping" sound, they're a practical solution for people who don't want a hole in their head. The "natural" feel of bone conduction is totally overrated if you're not a hardcore audiophile.
Andre Ojakäär
May 2, 2026 AT 23:40please... the BAHA 6 is barely an upgrade. they just slap a new version number on the bluetooth and call it a revolution while the actual transducer tech has been stagnant for years. absolute joke
Nila Sawyer
May 4, 2026 AT 20:02I am just so incredibly moved by how far medical technology has come to help people reconnect with the world around them! 🌟 Imagine the joy of a child born without an ear canal finally hearing their parents' voices for the first time because of a little bit of titanium! It's just so heartwarming and it gives me so much hope for the future of inclusive healthcare for everyone regardless of where they live! ✨💖
William Zhigaylo
May 6, 2026 AT 00:41The sheer incompetence of suggesting that a 10-15 dB loss is a negligible trade-off is staggering. One must possess an extraordinary level of ignorance to ignore the physiological impact of such a decrease in signal clarity. It is an insult to those who actually require precision in their auditory perception. Your failure to emphasize the gravity of this loss is utterly pathetic.
Jaclyn Vo
May 7, 2026 AT 20:15Omg and can we talk about the cleaning part?? 🙄 Rubbing alcohol every single day just to avoid an infection? No thank you! I'd rather be deaf than have a daily chore attached to my skull! 💅
Michael Deane
May 8, 2026 AT 07:33I don't care about the fancy magnetic stuff, we need to make sure this tech is being manufactured right here in the US and not outsourced to places that don't care about our security, because once you put a chip in your head you're basically a walking antenna for whoever owns the server, and it's high time we started prioritizing American medical sovereignty over these globalist corporate trends that just want to bleed us dry with $7000 implants!
Vijay AGarwal
May 10, 2026 AT 07:25THE COST IS ABSOLUTELY INSANE! Seven thousand dollars per ear?! It is a complete robbery of the patients! We are talking about a piece of titanium and a plastic processor, yet the pricing is scaled as if they are gifting you a new set of ears from a donor! It is a tragedy of the highest order!
Elle Torres Sanz
May 11, 2026 AT 20:00It's important to remember that not everyone has the same access to these surgeries globally. While this is great tech, the bridge between needing this and actually affording it is still too wide for many communities.
Beena Garud
May 12, 2026 AT 17:41One might contemplate the metaphysical shift in perception when the medium of sound changes from air to bone. It is not merely a biological bypass, but a fundamental alteration of how the individual integrates with the external environment, suggesting that our reality is shaped as much by the mechanism of reception as by the signal itself.
sachin singh
May 13, 2026 AT 09:29Very informative.