Diabetic Retinopathy Guide: Understanding Retinal Damage and Laser Treatment
 Apr, 17 2026
Apr, 17 2026
Imagine waking up and noticing a few strange dark spots floating in your vision. For many, this is the first real warning sign that something is wrong. The scary part? By the time you actually notice these changes, the damage to your eyes might already be significant. Diabetic Retinopathy is a complication of diabetes that damages the blood vessels inside the retina, the light-sensitive tissue at the back of the eye. It is the leading cause of blindness in working-age adults, but here is the good news: with early detection and the right treatment, most of this vision loss is preventable.
Quick Summary: What You Need to Know
- The Cause: Long-term high blood sugar weakens and damages retinal blood vessels.
- The Danger: It often has no symptoms until it is advanced, making annual screenings vital.
- The Stages: It progresses from mild leakages to the growth of abnormal, fragile blood vessels.
- The Fix: A combination of strict blood sugar control and medical interventions like laser treatment.
How Diabetes Actually Damages Your Eyes
To understand the damage, you first have to understand what the retina does. Think of your retina like the film in an old-school camera; it captures light and sends it to your brain. This process requires a massive, steady supply of oxygen and nutrients, delivered by a complex network of tiny blood vessels.
When you have diabetes, chronically high blood sugar levels act like a slow-acting poison to these vessels. Over time, the walls of the blood vessels weaken. This leads to microaneurysms, which are tiny bulges in the vessel walls. These weak spots can leak fluid or blood into the retina, causing it to swell. If the vessels get completely blocked, the retina doesn't get enough oxygen, and the eye tries to compensate by growing new blood vessels.
Here is the catch: these new vessels are not built well. They are fragile and prone to leaking or rupturing. When they bleed into the vitreous-the clear, gel-like substance filling your eye-it can create "floaters" or even cause a total retinal detachment, where the retina pulls away from the back of the eye. Once the photoreceptor cells die off due to lack of oxygen or scarring, the vision loss becomes permanent.
The Three Stages of Progression
Diabetic retinopathy doesn't happen overnight. It moves through stages, and knowing where you stand determines the urgency of treatment.
| Stage | What's Happening | Common Symptoms |
|---|---|---|
| Mild Nonproliferative | Tiny bulges (microaneurysms) form in blood vessels. | Usually none. |
| Moderate to Severe Nonproliferative | Vessels leak fluid (edema) or block blood flow. | Blurry vision, occasional floaters. |
| Proliferative (Advanced) | New, fragile blood vessels grow on the retina surface. | Dark spots, severe floaters, sudden vision loss. |
A specific and common complication is Diabetic Macular Edema (DME). The macula is the center of your retina responsible for the sharp, central vision you use for reading or recognizing faces. When fluid leaks specifically into this area, your central vision becomes blurry or wavy. About 1 in 15 people with diabetes will face this specific issue.
Recognizing the Red Flags
If you're waiting for your vision to change before you book an eye exam, you're playing a dangerous game. Most people have 20/20 vision while the early stages of retinopathy are actively destroying their retinal health. However, as the condition progresses, certain signs become impossible to ignore.
- Floaters: Dark streaks or spots that drift across your field of vision. This is often blood leaking into the vitreous.
- Blurry or Wavy Vision: This usually points to macular edema (swelling in the center of the eye).
- Night Blindness: Difficulty seeing in low light or while driving at night.
- Color Fade: Colors may seem less vibrant or distorted.
- Loss of Peripheral Vision: This happens in very advanced cases where the retina has detached or severe scarring has occurred.
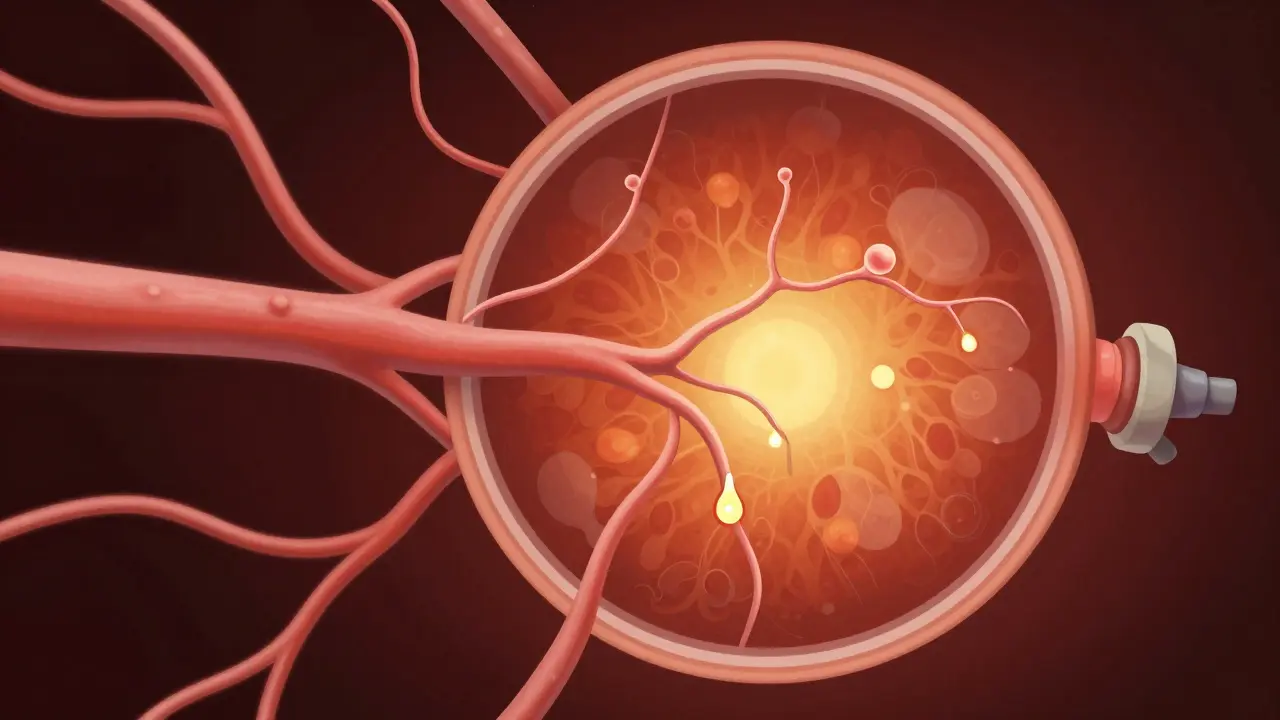
Laser Treatment: How It Works and What to Expect
When blood sugar management isn't enough to stop the damage, doctors turn to specialized procedures. One of the most established methods is laser photocoagulation, a process where a high-energy laser is used to treat the retina. But how does "burning" the eye actually help it?
The laser serves two main purposes depending on the stage of the disease. In the case of macular edema, the laser is used to seal the leaking blood vessels. By cauterizing the leak, the fluid is absorbed, and the swelling in the macula goes down, which clears up your central vision.
In the proliferative stage, the goal is different. The laser is used to shrink the abnormal, fragile blood vessels. By destroying these "leaky pipes," the doctor reduces the risk of a massive hemorrhage into the eye. In some cases, the laser is used to create a "fence" of burns around a detached retina to push it back into place.
While laser treatment is highly effective, it's rarely a standalone cure. It is typically used alongside modern medications, such as anti-VEGF injections, which stop the growth of those bad blood vessels in the first place. The real success comes from a "two-pronged attack": medical procedures to fix current damage and strict glycemic control to prevent new damage.
Reducing Your Risk: Beyond the Doctor's Office
You can't change how long you've had diabetes, but you can change how your eyes respond to it. The relationship between your A1C levels and your retinal health is direct. If your blood sugar is a rollercoaster, your blood vessels are the ones taking the ride.
Beyond blood sugar, keep an eye on your blood pressure. Hypertension puts extra pressure on the already weakened vessel walls in your eyes, making them more likely to burst or leak. Similarly, high cholesterol can contribute to the blockage of these tiny vessels.
If you are pregnant and have diabetes, you should be extra vigilant. Pregnancy can accelerate the progression of retinopathy, meaning your screening schedule might need to be more frequent. Finally, smoking is a major risk factor-it constricts blood vessels and reduces the oxygen reaching your retina, essentially speeding up the clock on vision loss.
The Path to Preserving Your Sight
The most important takeaway is this: diabetic retinopathy is treatable, but only if it's caught. If you have Type 1 or Type 2 diabetes, a comprehensive dilated eye exam is not optional-it is a necessity. During these exams, the doctor puts drops in your eyes to widen the pupil, allowing them to see the very back of the eye and spot microaneurysms before you ever see a floater.
If you're diagnosed, don't panic. Many patients who receive timely treatment have a 95% chance of preserving their vision. The key is consistency. Keep your appointments, manage your blood pressure, and stay on top of your glucose levels. Your sight is too valuable to leave to chance.
Can laser treatment completely cure diabetic retinopathy?
Laser treatment doesn't "cure" the underlying diabetes, but it can stop the progression of the disease. It seals leaking vessels and destroys abnormal ones to prevent blindness. However, because the underlying cause is high blood sugar, new damaged areas can still develop if diabetes isn't managed.
How often should I get my eyes checked if I have diabetes?
The general medical consensus, including guidelines from the NHS, is to have a comprehensive dilated eye exam at least once a year. If you are pregnant or have already shown signs of retinopathy, your doctor may suggest screenings every few months.
Does laser treatment hurt?
The procedure itself is generally painless because the laser targets the retina, which doesn't have pain receptors like your skin does. However, you may feel some pressure, and the bright lights can cause temporary glare or blurred vision immediately after the appointment.
What is the difference between retinopathy and macular edema?
Diabetic retinopathy is the broad term for all retinal blood vessel damage. Macular edema is a specific type of retinopathy where fluid builds up in the macula (the center of the retina), which specifically affects your sharp, central vision rather than your overall field of view.
Can I reverse the vision loss from retinopathy?
Some vision loss, particularly from macular edema, can be improved through laser treatment or injections. However, if the photoreceptor cells in the retina have died or if severe scarring has occurred, that part of the vision loss is usually permanent. This is why early detection is so critical.
Next Steps for Different Scenarios
- If you've never had a screening: Book a dilated eye exam immediately. Do not rely on a standard vision test (the one with the chart) as it does not check the health of the retina.
- If you've been diagnosed with mild retinopathy: Focus intensely on your Hemoglobin A1C levels and blood pressure. This is the stage where lifestyle changes can have the biggest impact on slowing the disease.
- If you are seeing floaters or blurred vision: Contact an ophthalmologist specializing in retinal diseases right away. These are signs that the condition may have progressed to the proliferative stage or that edema is present.
Aaron McGrath
April 18, 2026 AT 19:16Stop sleeping on your A1C levels! If you aren't aggressively optimizing your glycemic index and crushing those glucose spikes, you're basically inviting retinal degradation into your life.
Get your head in the game and hit the gym, optimize your macros, and stop letting your blood pressure redline! We need peak physiological performance to avoid these microaneurysms. No excuses, just results!
Tanya Rogers
April 20, 2026 AT 12:30One finds the simplistic correlation between biological malfunction and medical intervention quite quaint. To reduce the profound tragedy of losing one's sight to a mere set of "red flags" is to strip the human experience of its inherent entropy.
The medical establishment treats the eye as a camera, yet they ignore the ontological shift that occurs when a subject's perception of reality is fundamentally altered by pathology. Furthermore, the insistence on annual screenings suggests a desperate, almost pathetic attempt to quantify the inevitable decay of the flesh. It is an exercise in futility masquerading as preventative care. I find the clinical optimism presented here to be an affront to the nuanced reality of chronic illness. We are not merely machines to be tuned with lasers; we are witnesses to our own dissolution. The sterile nature of this guide ignores the existential dread that accompanies the first sighting of a floater. It is a superficial remedy for a systemic failure of the human form. Truly, the lack of philosophical inquiry into the nature of blindness within this text is staggering. One must wonder if the authors believe that a "two-pronged attack" solves the mystery of mortality. It is an amusingly naive perspective on the fragility of biological existence.
Olushola Adedoyin
April 21, 2026 AT 08:48The lasers are a trap! They want to burn your eyes so you can't see what they're really doing in those clinics! Big Pharma is just cooking our retinas for the insurance money!
Quinton Bangerter
April 21, 2026 AT 09:48Actually, the so-called "standard of care" for retinopathy is just a way to keep patients dependent on a cycle of injections and follow-ups. If you think a dilated exam is for your benefit, you're just falling for the narrative. They just want a better view of your vulnerabilities.
Cynthia Didion
April 22, 2026 AT 00:55American medicine is the only gold standard. Anywhere else, you'd be blind by fifty.
Venkatesh Venky
April 23, 2026 AT 11:07Let's just focus on staying positive and following the doctor's advice to keep our vision clear. Using anti-VEGF therapies combined with steady glucose monitoring can really make a difference for everyone!
Ms. Sara
April 24, 2026 AT 14:42It's so important to remind people that blood pressure management is just as critical as sugar levels here. I've seen so many patients ignore their hypertension and then wonder why their retinopathy progressed so rapidly. Please, take care of your whole heart to save your eyes.