Birth Control Pills: Effectiveness, Side Effects, and Drug Interactions Guide
 May, 8 2026
May, 8 2026
For decades, the daily ritual of taking a small pill has been the cornerstone of family planning for millions of women. But does that tiny tablet actually do what it promises? The short answer is yes, but with a major caveat: you have to take it perfectly. Birth control pills, also known as oral contraceptives, are hormonal medications designed to prevent pregnancy by regulating your menstrual cycle. While they are the most commonly used reversible contraceptive method in the United States, their success hinges entirely on user adherence. If you miss a dose or take it at erratic times, the protection drops significantly. Understanding how these pills work, what goes wrong when they interact with other substances, and the real-world statistics behind their effectiveness is crucial for making an informed choice. This guide breaks down the science, the risks, and the practical realities of using oral contraceptives in 2026.
How Birth Control Pills Work and Their Types
To understand why pills fail or cause side effects, you first need to know what’s inside them. There are two primary categories of oral contraceptives available today, each functioning differently within your body.
Combined Oral Contraceptives (COCs) contain two types of hormones: estrogen and progestin. These hormones work together to stop ovulation-the release of an egg from the ovaries. Without an egg, sperm has nothing to fertilize. Most modern COCs contain low doses of ethinyl estradiol, typically between 20 and 35 micrograms (μg). Early versions in the 1960s contained massive doses of up to 10,000 μg, which led to serious health risks. Today’s formulations are much safer, with many experts considering pills containing 30 μg of estrogen and levonorgestrel as having the safest cardiovascular risk profile.
The second type is Progestin-Only Pills (POPs), often called the 'mini-pill'. These contain only progestin, usually norethindrone at 0.35 mg per tablet. Unlike COCs, POPs do not always stop ovulation. Instead, they thicken cervical mucus to block sperm and thin the lining of the uterus to prevent implantation. A newer formulation, Slynd®, uses 4 mg of drospirenone and offers a slightly wider window for missed doses compared to traditional mini-pills.
Choosing between these depends on your health history. For instance, if you have a history of blood clots or high blood pressure, doctors often recommend POPs because they lack estrogen, which can increase clotting risks.
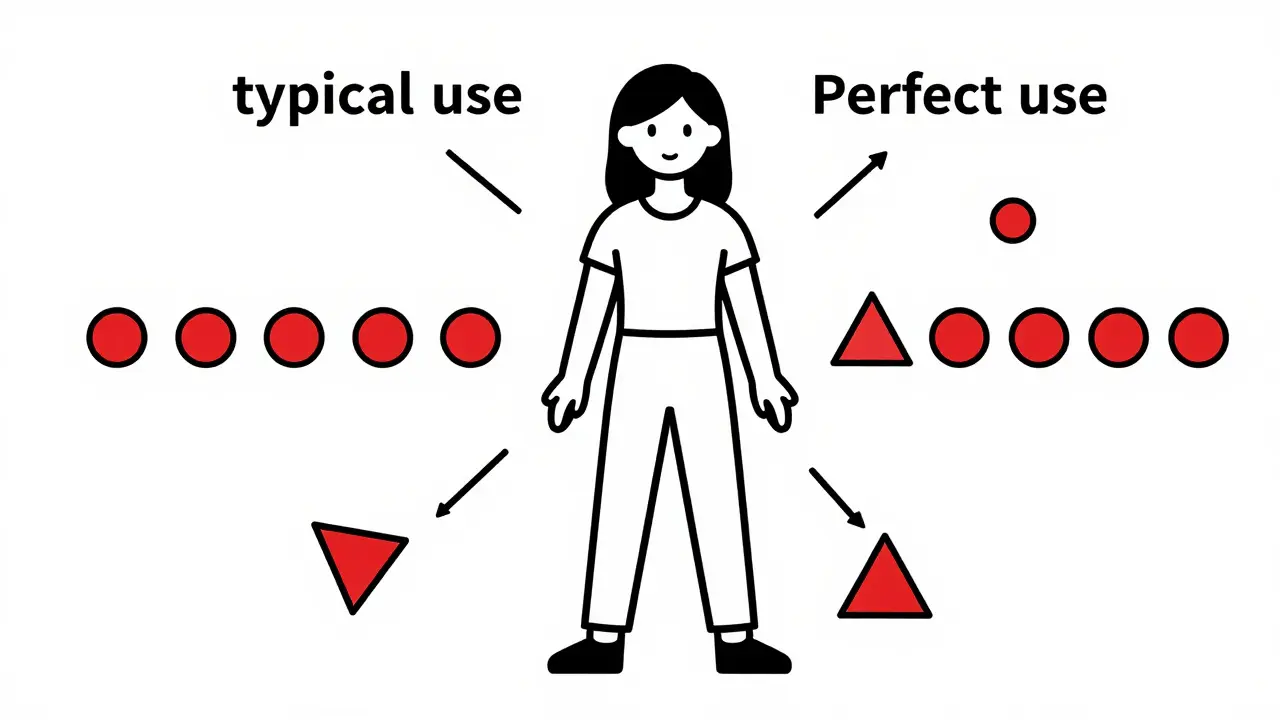
Effectiveness: Perfect Use vs. Typical Use
This is where the numbers get tricky, and why many people feel misled by marketing materials. You will often see claims that birth control pills are "99% effective." That number is true only under perfect use conditions-meaning you take the pill at the exact same time every single day, without ever missing a dose or vomiting shortly after taking it.
In the real world, life happens. According to data from the CDC and the Guttmacher Institute, the typical use effectiveness of birth control pills drops to approximately 93%. This means that out of 100 women who rely on the pill for one year, about seven will experience an unintended pregnancy. The discrepancy between perfect and typical use is largely due to human error. Missing even one pill can disrupt the hormonal balance enough to allow ovulation to occur.
Compare this to Long-Acting Reversible Contraceptives (LARCs) like IUDs or implants. These methods don’t require daily action. An IUD has a failure rate of less than 1%, and an implant is over 99% effective regardless of user behavior. For younger users, particularly those under 21, the risk of pregnancy with short-acting methods like pills is nearly twice as high as for older users, primarily due to consistency challenges.
| Method | Perfect Use Failure Rate | Typical Use Failure Rate | User Action Required |
|---|---|---|---|
| Combined Oral Contraceptives (COCs) | 0.1% - 1% | 7% - 9% | Daily pill intake |
| Progestin-Only Pills (POPs) | 0.3% - 1% | 5% - 9% | Daily pill intake (strict timing) |
| Hormonal IUD | 0.1% - 0.2% | 0.1% - 0.4% | Annual check-up |
| Implant (Nexplanon) | 0.05% | 0.05% | Replacement every 3-5 years |
Side Effects and Health Benefits
Like any medication, birth control pills come with a list of potential side effects. For many, these are minor and fade after the first few months as the body adjusts. Common complaints include nausea, breast tenderness, headaches, and mood swings. Some women experience breakthrough bleeding-spotting between periods-which is especially common with progestin-only pills.
However, there are more serious risks to consider. The most significant concern with combined oral contraceptives is the increased risk of blood clots, stroke, and heart attack. This risk is higher in women who smoke, are over age 35, or have underlying cardiovascular issues. Modern low-dose pills have reduced this risk considerably compared to earlier generations, but it never disappears entirely.
On the flip side, birth control pills offer substantial non-contraceptive health benefits. Epidemiological studies show that long-term use of COCs can reduce the risk of ovarian cancer by up to 27% and endometrial cancer by 50%. These protective effects can last for up to 20 years after stopping the pill. Additionally, certain formulations containing drospirenone are FDA-approved to treat acne and hirsutism (excess hair growth) in women aged 14 and older. They also help regulate menstrual cycles and reduce symptoms of premenstrual syndrome (PMS).
Drug Interactions That Compromise Protection
One of the most overlooked aspects of birth control pill safety is drug interactions. Certain medications can interfere with the liver enzymes that metabolize estrogen and progestin, causing hormone levels in your blood to drop below the threshold needed to prevent pregnancy.
The most well-known offenders are enzyme-inducing drugs. These include:
- Anticonvulsants: Medications like carbamazepine, phenytoin, and topiramate (at higher doses) used for epilepsy or migraines.
- Antibiotics: Specifically rifampin and rifabutin, used to treat tuberculosis. Note that most common antibiotics (like amoxicillin) do not affect pill efficacy, but diarrhea caused by antibiotics can impair absorption.
- HIV Medications: Protease inhibitors and non-nucleoside reverse transcriptase inhibitors.
- Herbal Supplements: St. John’s Wort is a potent enzyme inducer that can significantly reduce contraceptive effectiveness.
If you are prescribed any of these medications, your doctor should advise you to switch to a non-hormonal method, such as a copper IUD or condoms, or to add backup protection. Always inform your pharmacist and healthcare provider that you are on hormonal contraception before starting any new treatment.
Practical Tips for Maximizing Effectiveness
Since typical use failure rates are driven by human error, building a robust routine is your best defense. Here are actionable steps to ensure your pill works as intended:
- Set a Daily Alarm: Take your pill at the same time every day. For progestin-only pills, timing is critical; being more than three hours late can compromise protection. For combined pills, you have a slightly wider window, but consistency still matters.
- Use Backup During the First Week: When you start a new pack or switch brands, the pill may not be fully effective for the first seven days. Use condoms during this period.
- Know What to Do If You Miss a Pill: If you miss one combined pill, take it as soon as you remember and continue with the rest of the pack. If you miss two or more, consult your package insert or doctor immediately, as you may need emergency contraception and backup methods for the next week.
- Monitor Your Body: Keep track of any unusual symptoms like severe leg pain, chest pain, or sudden vision changes, which could signal a blood clot or stroke. Seek immediate medical attention if these occur.
Remember, birth control pills do not protect against sexually transmitted infections (STIs). Using condoms alongside the pill is highly recommended, especially if you have multiple partners or are unsure of your partner’s status. This dual protection strategy safeguards both your reproductive choices and your overall sexual health.
When to Consider Alternatives
While birth control pills are convenient, they aren’t the right fit for everyone. If you struggle with daily routines, have a history of blood clots, smoke heavily, or are looking for a "set it and forget it" solution, you might benefit from exploring Long-Acting Reversible Contraceptives (LARCs). IUDs and implants offer superior effectiveness with minimal user involvement. Discussing your lifestyle, health history, and future fertility plans with a healthcare provider can help you choose the method that aligns best with your needs.
Are birth control pills 100% effective?
No, birth control pills are not 100% effective. With perfect use, they are about 99% effective, meaning less than 1 in 100 women will get pregnant in a year. However, with typical use (which includes missed or late pills), effectiveness drops to around 93%, resulting in about 7 pregnancies per 100 women annually.
Can antibiotics make birth control pills ineffective?
Most common antibiotics, such as amoxicillin, do not reduce the effectiveness of birth control pills. However, specific antibiotics like rifampin and rifabutin, used for tuberculosis, can significantly lower hormone levels. Additionally, if antibiotics cause severe diarrhea, your body may not absorb the pill properly, increasing the risk of pregnancy.
What are the most common side effects of combined oral contraceptives?
Common side effects include nausea, breast tenderness, headaches, mood changes, and breakthrough bleeding. These symptoms often improve after the first three months of use. Serious but rare side effects include blood clots, stroke, and heart attack, particularly in smokers over age 35.
Do birth control pills protect against STIs?
No, birth control pills do not provide any protection against sexually transmitted infections (STIs) like HIV, chlamydia, or gonorrhea. To protect against STIs, you must use barrier methods such as condoms in addition to hormonal contraception.
How quickly does fertility return after stopping birth control pills?
Fertility returns very quickly after stopping combined oral contraceptives. According to CDC data, 97% of women experience spontaneous menstruation within 90 days of discontinuing the pill. Many women can conceive almost immediately, so if you wish to avoid pregnancy, start another method right away.
What should I do if I miss a birth control pill?
If you miss one combined pill, take it as soon as you remember and continue with your regular schedule. If you miss two or more pills, take the most recent missed pill immediately, discard any others, and use backup contraception like condoms for the next seven days. For progestin-only pills, being more than three hours late requires backup protection for 48 hours.